Owner
U
UntitledVerification
Tags
Prostate
1. What it is (core identity)
- Partly glandular + partly fibromuscular male internal genital organ.
- Lies below the bladder and above the urogenital diaphragm.
- Proximal urethra (prostatic urethra) traverses its full length.
- Size: broader than long, ~ 4 × 3 × 2 cm.
- Female homologue: paraurethral (Skene’s) glands.
- Function: contributes ~30% of seminal fluid (majority from seminal vesicles).
2. External anatomy (surfaces & poles → relations)
- Base (upper surface)
- Fused to bladder neck.
- Perforated by urethra entering at the internal meatus.
- Apex (lower, blunt)
- Lowest part.
- Prostatic urethra exits anteriorly to become membranous urethra, surrounded by sphincter urethrae.
- Anterior surface
- Forms posterior wall of retropubic (Retzius) space.
- Anchored to pubic bones via puboprostatic ligaments.
- Inferolateral surfaces
- Clasped by pubourethralis parts of levator ani.
- Posterior surface
- Anterior to lower rectum, separated by rectovesical (Denonvilliers’) fascia.
- Ejaculatory ducts
- Pierce posterior surface just below bladder, pass obliquely ~2 cm, open into prostatic urethra midway down.
- Prostatic ducts also open into this same urethral region.
3. Capsules & venous plane (surgical logic)
- True capsule: thin, strong connective tissue at gland periphery.
- False capsule: condensation of pelvic fascia outside true capsule.
- Between capsules: prostatic venous plexus (important bleeding plane).
4. Histology (why it behaves the way it does)
- Acini of variable size/shape embedded in fibromuscular stroma
(smooth muscle + connective tissue) → characteristic feature.
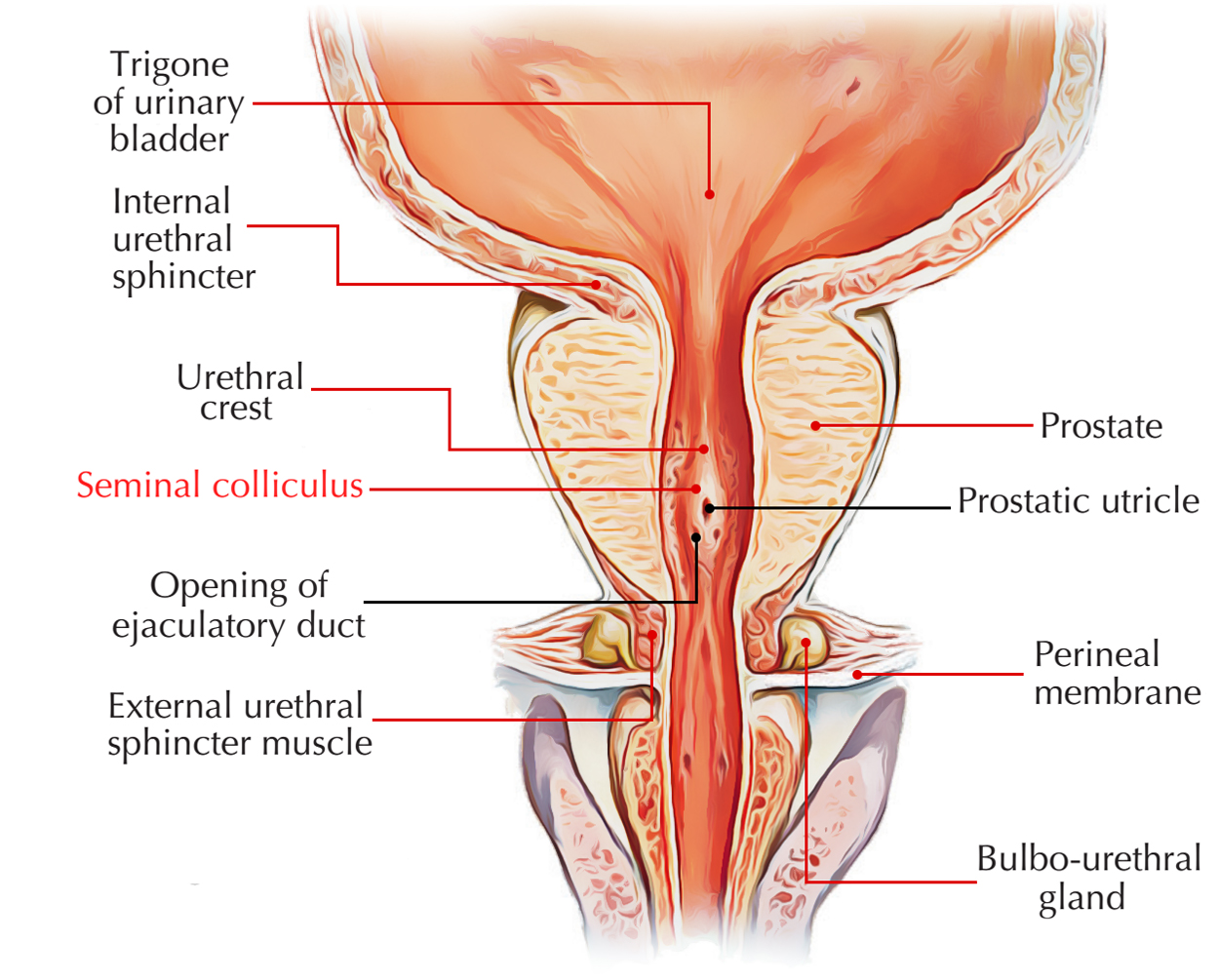
5. Prostatic urethra (3–4 cm) — exact course & landmarks
- Passes closer to anterior than posterior surface.
- Course:
- From internal meatus → downwards & backwards
- Bends at mid-length
- Continues downwards & forwards
- Exits anterior aspect of apex.
- Posterior wall features:
- Urethral crest (midline ridge) along most of length.
- Prostatic sinuses: shallow depressions on either side.
- Seminal colliculus (verumontanum): midline rounded eminence at mid-length.
- Prostatic utricle (remnant of fused Müllerian ducts) opens on the verumontanum.
- Ejaculatory ducts open on either side of utricle.
- Preprostatic (proximal) part:
- Surrounded by smooth muscle cylinder (extension of bladder neck circular muscle).
- Contracts during ejaculation → prevents seminal regurgitation into bladder.
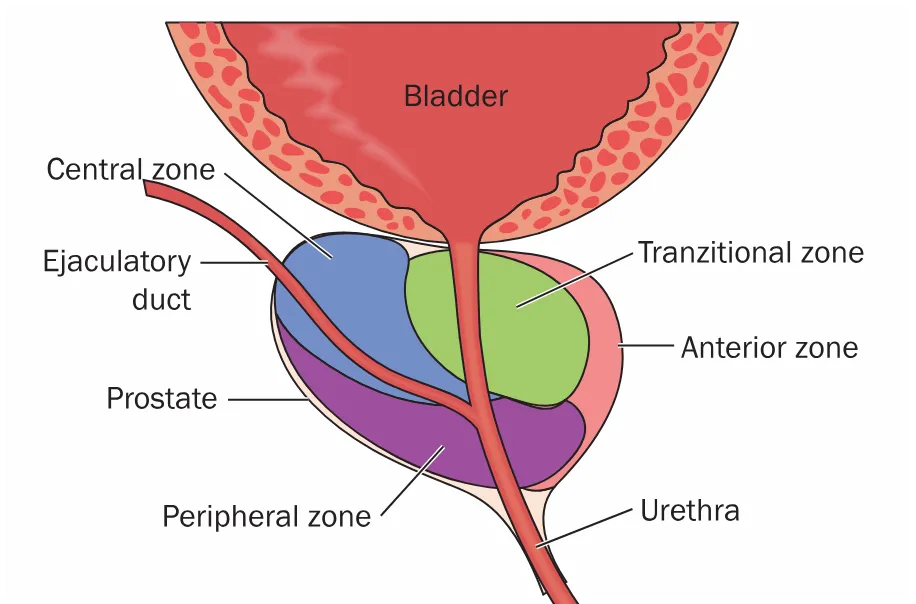
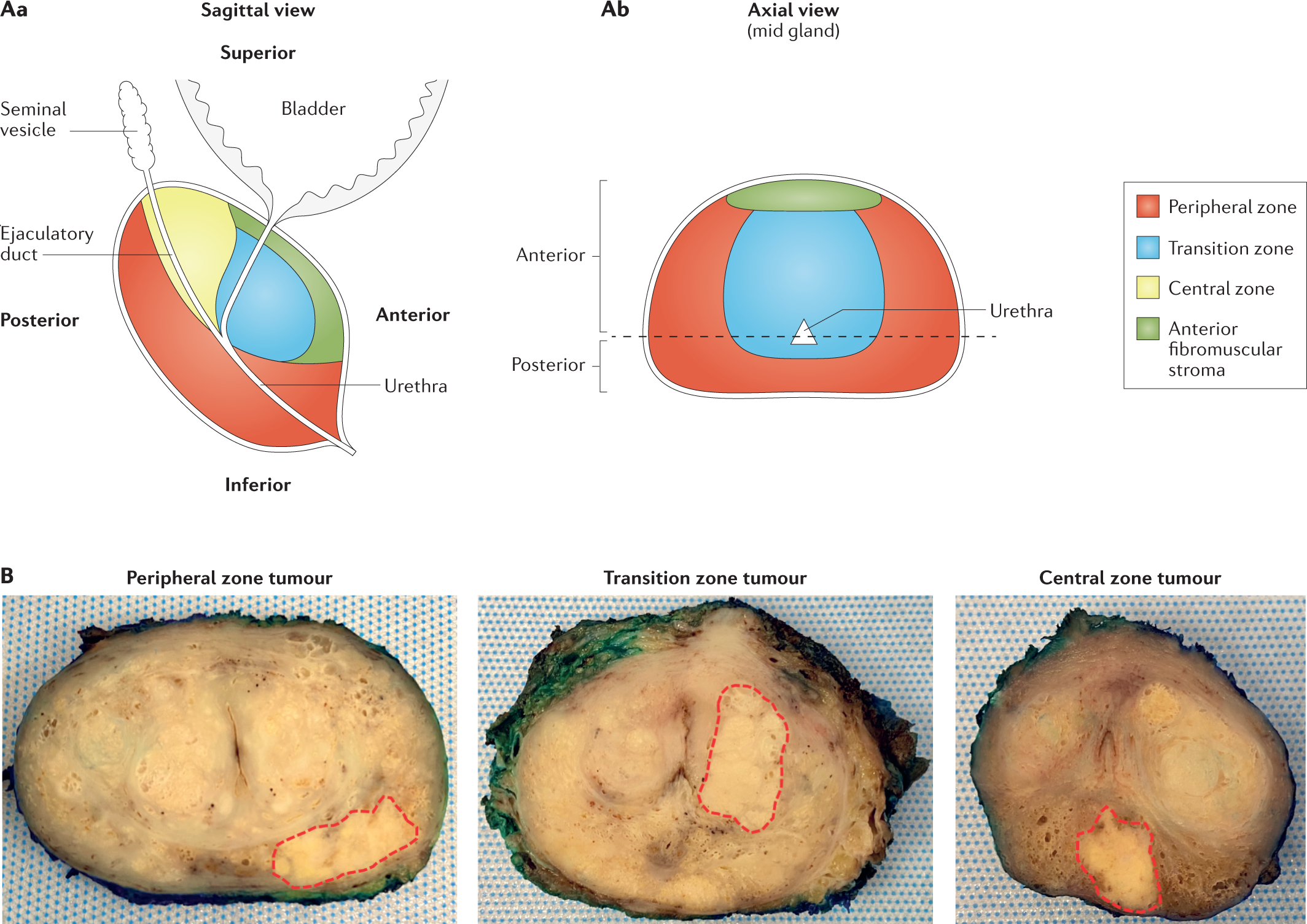
6. Zonal anatomy (modern, disease-critical)
- Peripheral zone (~70%)
- Surrounds central zone posteriorly & inferiorly.
- Does not reach the base; forms lower part of gland.
- Primary site for carcinoma.
- Central zone (~20%)
- Wedge-shaped; forms base, apex at verumontanum.
- Surrounds ejaculatory ducts.
- Rarely diseased.
- Transition zone (~5%)
- Around distal preprostatic urethra, just proximal to apex of central zone.
- Ducts open on verumontanum, above peripheral zone ducts.
- Benign prostatic hyperplasia (BPH) originates here → expansion compresses peripheral zone.
7. Anterior prostate (composition & neighbors)
- Very little glandular tissue anterior to urethra.
- Predominantly fibromuscular.
- Overlapped:
- Above by detrusor muscle of bladder.
- Below by striated external urethral sphincter.
8. Blood supply (arteries → veins → drainage logic)
- Arteries:
- Prostatic branch of inferior vesical artery (main).
- Small branches from middle rectal and internal pudendal arteries.
- Veins:
- Form plexus between true & false capsules.
- Join vesicoprostatic plexus at bladder–prostate groove.
- Receives deep dorsal vein of penis.
- Drains posteriorly to internal iliac veins.
9. Lymph drainage
- Mainly to internal iliac nodes.
- A few channels to external iliac nodes.
10. Nerve supply (function-linked)
- Glandular acini: parasympathetic (cholinergic) via pelvic splanchnic nerves → inferior hypogastric plexus (secretion).
- Fibromuscular stroma: sympathetic (adrenergic) via inferior hypogastric plexus → contraction during ejaculation (emptying).
11. Development (zone-specific origin)
- Endodermal urogenital sinus (pelvic part) → lateral epithelial buds → acini of peripheral & transition zones.
- Dorsal outgrowths above mesonephric duct entry → central zone acini.
- Fibromuscular stroma → from surrounding mesenchyme.
12. Surgical approaches (anatomy → safety rules)
- BPH: usually transurethral resection (TURP).
- Resection kept above the verumontanum → protects external urethral sphincter (which lies distal).
- Carcinoma:
- Radical prostatectomy via retropubic (suprapubic) approach, laparoscopic, or perineal route.
- Bladder neck anastomosed to membranous urethra.
One-line exam lock
- BPH = transition zone, Carcinoma = peripheral zone, continence protected by staying above verumontanum.
VAS DEFERENS & SEMINAL VESICLE — LOGIC MAP
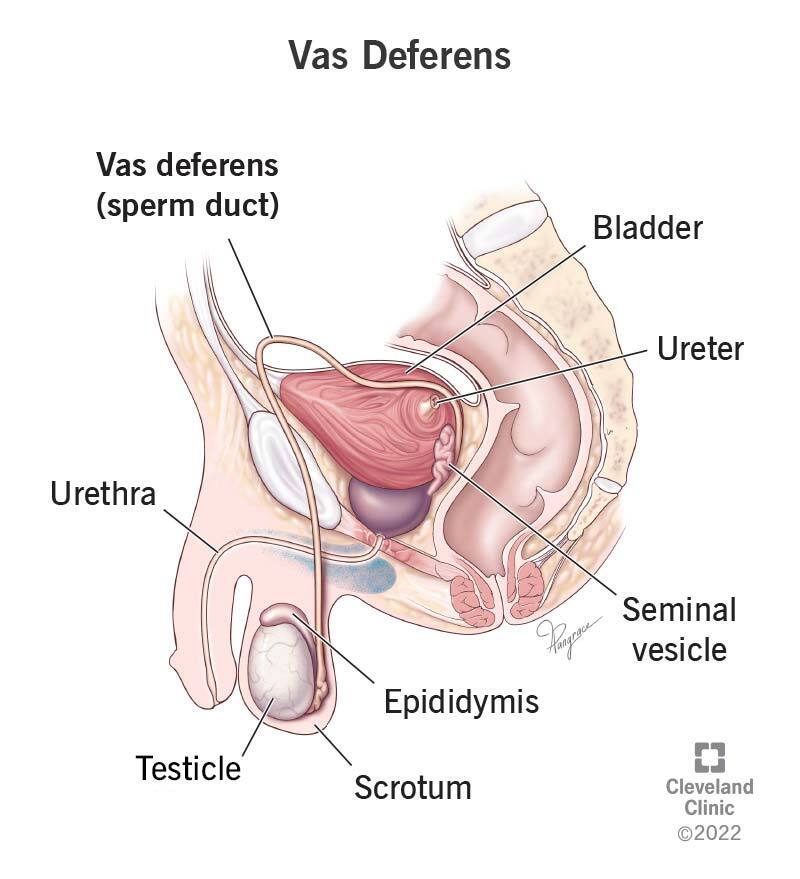


1. Vas deferens — course explained as a journey
Origin
- Continuation of the epididymis.
- Enters abdomen via the deep inguinal ring.
Pelvic course (step-by-step logic)
At deep inguinal ring
- Hooks around:
- Interfoveolar ligament
- Inferior epigastric artery
Immediately after entering pelvis
- Crosses:
- External iliac artery
- External iliac vein
- Obliterated umbilical artery
- Obturator nerve, artery, and vein
- Lies on obturator fascia.
- Important relationship:
- No structure intervenes between vas and peritoneum → directly subperitoneal.
Approaching bladder
- Curves medially and forwards.
- Crosses above the ureter
→ classic exam line: “Water (ureter) under the bridge (vas).”
Behind bladder
- Meets its fellow.
- Both turn downwards side by side.
- Each duct dilates fusiformly → ampulla of vas deferens.
2. Ampulla of vas deferens — purpose & relations
- Function:
- Storehouse of spermatozoa.
- Physiology:
- Proximal vas absorbs fluid from seminiferous tubules.
- Vas itself contributes very little to seminal fluid volume.
- Relations:
- Ampullae lie parallel and medial to seminal vesicles.
- Termination:
- Lower end loses thick muscle wall.
- Joins duct of seminal vesicle → ejaculatory duct.
3. Ejaculatory duct — final pathway
- Formed by:
- Ampulla of vas deferens
- Duct of seminal vesicle
- Course:
- Passes obliquely through the prostate.
- Opens on:
- Verumontanum (in prostatic urethra).
4. Seminal vesicle — structure, position, function
Structure
- Thin-walled, elongated sac
- Like a lobulated blind-ending tube
- Highly folded on itself
Function
- Produces ~60% of seminal fluid (major contributor).
Position & relations
- Applied to base of bladder, above prostate.
- Rectovesical fascia lies posteriorly.
- Upper ends:
- Just covered by peritoneum of rectovesical pouch.
- Each seminal vesicle lies:
- Lateral to the ampulla of its own vas deferens.
- At lower end:
- Duct joins vas → ejaculatory duct.
5. Blood supply (high-yield vessels)
Vas deferens
- Artery to vas:
- Branch of superior vesical artery
- Sometimes from inferior vesical artery
- Accompanies vas to lower pole of epididymis.
- Anastomoses with testicular artery.
Seminal vesicles
- Supplied by branches from:
- Inferior vesical artery
- Middle rectal artery
6. Lymphatic drainage
- Lymphatics follow vessels.
- Drain to nearest iliac lymph nodes.
7. Nerve supply — exam-critical physiology
- Smooth muscle of:
- Vas deferens
- Seminal vesicles
- Supplied by:
- Inferior hypogastric plexus
- Fibres are mainly:
- Sympathetic motor fibres
- From first lumbar ganglion
- Via hypogastric plexuses
Clinical consequence
- Division of these nerves →
- Sterility
- Paralysed smooth muscle
- No contraction → no emission or ejaculation
8. Histological structure (compare vas vs vesicle)
Vas deferens
- Very thick muscular wall
- Small lumen
- Muscle layers:
- Inner longitudinal
- Middle circular
- Outer longitudinal
- Mucosa:
- Columnar epithelium
- With stereocilia (elongated microvilli)
Seminal vesicle
- Muscle coat thinner than vas.
- Single tube but highly convoluted →
- Appears as multiple tubules in section.
- Mucosa:
- Very folded
- Gland-like appearance.
- Epithelium:
- Columnar
9. Development (embryology lock)
- Vas deferens:
- Major derivative of mesonephric (Wolffian) duct.
- Seminal vesicle:
- Develops as a diverticulum from mesonephric duct
- Forms at back of prostate.
One-line exam synthesis
The vas deferens, a thick-walled muscular derivative of the mesonephric duct, crosses above the ureter to form an ampulla behind the bladder, which joins the seminal vesicle duct to form the ejaculatory duct that traverses the prostate to open on the verumontanum, while seminal vesicles provide the bulk of seminal fluid.