Owner
U
UntitledVerification
Tags
AVASCULAR_PELVIC_SPACES.pdf3.8 MiB
okabyashi,latzko-https://www.youtube.com/watch?v=WMeKLGtsHHM

Feature | Medial Paravesical Space (MPS) | Lateral Paravesical Space (LPS) |
Divided by | → Medial to obliterated umbilical artery | → Lateral to obliterated umbilical artery |
Also called | Medial compartment | Obturator space |
Medial relation | Bladder | Obliterated umbilical artery |
Lateral relation | Obliterated umbilical artery | External iliac vessels |
Main contents | Loose areolar tissue | Obturator nerve, artery, vein + lymphatics |
Floor | Iliococcygeus + pubocervical fascia | Same |
Surgical use | • Bladder mobilization • Ureteric surgery • Anterior exenteration | • Pelvic lymphadenectomy • Burch colposuspension • Paravaginal repair |
Oncologic relevance | Access to bladder / ureter | Node dissection zone |
Key risk | Bladder / ureter injury | Obturator nerve + Corona mortis bleeding |
Opened until | Levator ani | Obturator nerve |
Feature | Latzko’s Space (Lateral PRS) | Okabayashi’s Space (Medial PRS) |
Position | Lateral to ureter / mesoureter | Medial to ureter / mesoureter |
Also called | Lateral pararectal space | Medial pararectal space |
Medial boundary | Ureter + mesoureter | Rectum+rectal pillers |
Lateral boundary | Internal iliac artery | Ureter + mesoureter |
Ventral boundary | Cardinal ligament | Cardinal ligament |
Dorsal boundary | Presacral fascia / sacrum | Presacral fascia / sacrum |
Dividing structure (practical) | Ureter / hypogastric nerve | Ureter / hypogastric nerve |
Main contents | Loose areolar tissue | Lateral ligament of rectum + middle rectal vessels |
Key exposure | Uterine artery origin | Hypogastric nerve + pelvic plexus |
Primary surgical use | • Pelvic lymphadenectomy • Internal iliac ligation • Radical hysterectomy | • Nerve-sparing radical hysterectomy • Deep endometriosis • Ureter mobilization |
Main purpose | Vascular access | Nerve preservation |
Important risk | Internal iliac vein / ureter | Pelvic plexus / middle rectal artery |
Feature | Yabuki Space |
Described by | Yoshihiko Yabuki (2000) |
Also called | Fourth space / Okabayashi paravaginal space |
Location | Between ureter and cranial vesico-uterine ligament |
Alternative description | Between lateral vagina & caudal vesico-cervical ligament |
Opened after | Dissection of cranial vesico-uterine ligament |
Medial relation | Bladder / vagina |
Lateral relation | Ureter |
Key contents | Pelvic splanchnic nerves (bladder innervation) |
Dissection direction | Toward vesicoureteric junction |
Main surgical role | Nerve-sparing radical hysterectomy |
Functional importance | Preserves bladder autonomic function |
High-risk injury | Pelvic splanchnic nerves → postoperative urinary dysfunction |
Feature | Retzius Space (Cavum Retzii) |
Named after | Anders Retzius |
Type of space | Extraperitoneal potential space |
Ventral boundary | Pubic symphysis |
Dorsal boundary | Bladder + parietal peritoneum |
Cranial boundary | Transversalis fascia |
Caudal boundary | Urethra, bladder neck, pubocervical fascia |
Lateral boundary | Arcus tendineus fascia pelvis (over obturator internus) |
Medial contents | Bladder / urethra |
Important structures | Pubourethral ligament, urachus (median umbilical ligament) |
Major venous structure | Veins of Santorini (retropubic venous plexus) |
Relationship to paravesical space | Paravesical spaces lie laterally |
Nature | Not a single cavity → multiple fascial planes |
Surgical access landmark | Median + medial umbilical ligaments |
Main urogynecologic uses | • Burch colposuspension • Retropubic TVT • Anterior compartment repair |
Gynecologic uses | • Bladder endometriosis |
Oncologic uses | • Anterior exenteration • Anterior peritonectomy |
Major risks | Bladder injury + Santorini plexus bleeding |
Space (All 9) | Class | Key “Finder” Landmark | Core Boundaries (must-know) | Direct Connections (how you “move” between spaces) | Main Uses (ObGyn / Urogyn / Obstetrics) | Main Danger / “Exam Trap” |
7) Vesicocervical Space | Median | “Anterior cul-de-sac axis” between bladder & cervix | Anterior: bladderPosterior: pubocervical fascia + cervix (upper)Lateral: cranial vesicouterine ligamentCranial: peritoneal reflection between bladder dome & low uterine segment | ↔ Vesicovaginal space (its inferior extension; same longitudinal axis)↔ Links medially with MPS during bladder mobilisation and with vesicouterine ligament planes | All hysterectomies (abdominal/laparoscopic/robotic/vaginal), radical hysterectomy (deeper dissection), nerve-sparing work in DIE/cancer | Must stay above pubovesical fascia: “fat belongs to bladder”; lateral dissection risks ureter/vessels in vesicouterine ligament |
8) Vesicovaginal Space | Median | Inferior continuation of vesicocervical; near trigone | Anterior: trigone of bladderPosterior: pubocervical fascia + vagina (inferior)Lateral: cranial vesicouterine ligamentCranial: same peritoneal reflection as aboveCaudal: junction of proximal & middle thirds of urethra; below this vagina and urethra fuse | ↔ Vesicocervical space (continuous)↔ Links to MPS/Yabuki planes laterally/at ligament–ureter interface in nerve-sparing dissections | Urogyn: vesicovaginal/ureterovaginal fistula repair, cystocele surgery, sacrocolpopexy/hysterocolpopexyGyn/Oncogyn: hysterectomy, radical hysterectomy (remove upper vagina), nerve-sparing DIE/cancer, vaginal cuff resectionObs: CS, cesarean hysterectomy, cerclage, CS scar ectopic excision | Cranial vesicouterine ligament contains uterine artery + superficial uterine vein + ureteric branch + superior vesical vein + cervicovesical vessels; lateral dissection → ureter/vessel injury |
9) Rectovaginal Space | Median | Posterior cul-de-sac plane; between rectum & vagina | Anterior: posterior vaginal wallPosterior: anterior rectal wallLateral: uterosacral ligaments (cranial) + rectovaginal ligament (caudal)Cranial: pouch of Douglas reflectionCaudal: levator ani | ↔ Links with Okabayashi/Latzko planes in deep endometriosis approaches (lateral-to-medial technique after opening both pararectal spaces described)↔ Continues posteriorly toward presacral planes depending on approach | Gyn/Oncogyn: radical hysterectomy, pelvic adhesions, deep endometriosis, rectovaginal fistula repairUrogyn: sacrocolpopexy, uterosacral suspensionVaginal route: rectocele repair | Rule: “fat belongs to rectum”; bleeding from middle rectal vessels/vaginal veins/presacral veins; rectal injury if wrong plane |
10) Presacral / Retrorectal Space | Median | Promontory + common iliac vessels + ureters; “holy plane” concept (inter-fascial) | Anterior: mesorectal fascia/rectumPosterior: anterior longitudinal ligament + sacral promontory + sacrumLateral: right common iliac artery/ureter; left common iliac vein/ureter; hypogastric fascia (medial fibers of USL)Cranial: rectosigmoid peritoneal reflectionCaudal: pelvic floorAlso divided by Waldeyer’s fascia into superior/inferior retrorectal space | ↔ Posterior continuation from pararectal spaces (Latzko/Okabayashi) toward sacral planes↔ Links superiorly to para-aortic lymphadenectomy initiation planes↔ Links to sacrocolpopexy “prelumbar/presacral” access | Oncogyn: TME for ovarian cancer infiltrating rectum; start para-aortic lymphadenectomyGyn: bowel endometriosis surgery (approach choice: inter-fascial vs trans-mesorectal described)Urogyn: sacrocolpopexyGyn: presacral neurectomy | High risk early: common iliac vessels, IMA, ureters; hard-to-control bleeding from middle sacral vessels; protect superior hypogastric plexus + hypogastric nerves |
1️⃣ Big picture: what are pelvic spaces?
- Pelvic spaces = potential spaces
- Created by pelvic fascia splitting
- Usually avascular or relatively bloodless
- Used to:
- Mobilize organs
- Control hemorrhage
- Avoid nerves & ureters
- Perform radical pelvic surgery safely
2️⃣ Classification (exam-friendly)
▶️ Anterior pelvic spaces
- Retropubic space (Space of Retzius)
- Vesicouterine space
▶️ Posterior pelvic spaces
- Rectouterine space (Pouch of Douglas)
- Presacral (retrorectal) space
▶️ Lateral pelvic spaces (MOST IMPORTANT surgically)
- Paravesical space
- Pararectal space
- Medial pararectal space (Okabayashi)
- Lateral pararectal space (Latzko)
3️⃣ Individual spaces — boundaries, relations, surgical value
🟦 Retropubic space (Space of Retzius)


Location
Between pubic symphysis and urinary bladder
Boundaries
- Anterior → Pubic symphysis
- Posterior → Bladder
- Superior → Peritoneal reflection
- Inferior → Endopelvic fascia
Contents
- Loose areolar tissue
- Dorsal venous complex (important in males)
Surgical importance
- Entry point for:
- Burch colposuspension
- Retropubic sling (TVT)
- Bladder mobilization
- Avoids peritoneal breach
⚠️ Injury risk: bladder perforation, venous bleeding
🟦 Vesicouterine space


Location
Between bladder and uterus/cervix
Boundaries
- Anterior → Bladder
- Posterior → Cervix & lower uterine segment
- Superior → Peritoneal fold
- Inferior → Vaginal vault
Surgical importance
- Opened in:
- Abdominal hysterectomy
- Caesarean section
- Allows safe bladder reflection
⚠️ In repeat CS: adhesions obliterate this space → bladder injury risk
🟦 Rectouterine space (Pouch of Douglas)
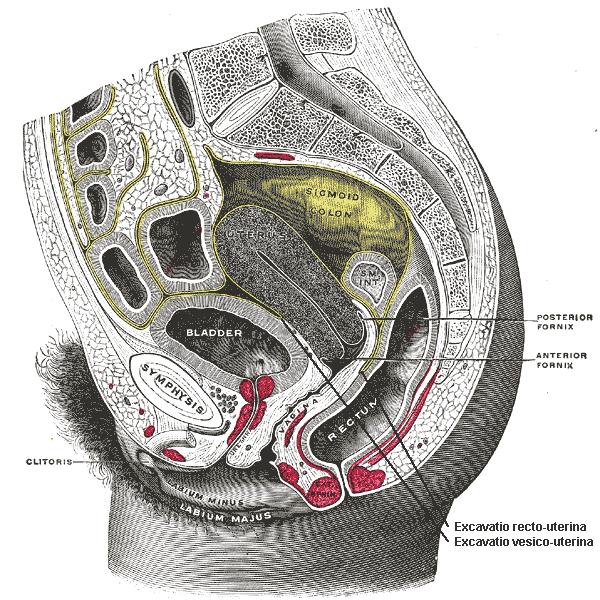


Location
Between posterior vaginal wall / uterus and rectum
Boundaries
- Anterior → Posterior fornix, cervix
- Posterior → Rectum
- Lateral → Uterosacral ligaments
Clinical importance
- Lowest peritoneal point → fluid collection
- Accessed via posterior colpotomy
Surgical relevance
- Drainage of pelvic abscess
- Endometriosis surgery
- Posterior vaginal wall procedures
🟦 Presacral (retrorectal) space



Location
Between rectum and sacrum
Boundaries
- Anterior → Rectum
- Posterior → Presacral fascia & sacrum
- Lateral → Iliac vessels
- Inferior → Pelvic floor
Contents
- Presacral venous plexus (⚠️ dangerous!)
Surgical importance
- Total mesorectal excision (TME)
- Rectal cancer surgery
⚠️ Presacral bleeding is:
- Profuse
- Difficult to control
- Potentially fatal
4️⃣ Lateral pelvic spaces (CORE EXAM + SURGERY)
🟩 Paravesical space

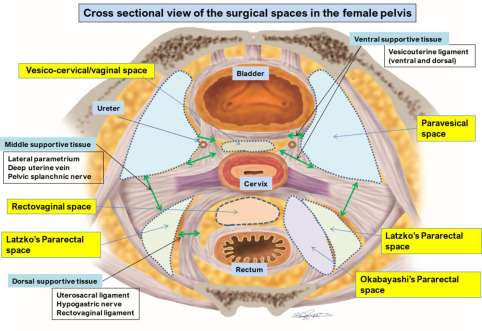

Location
Lateral to bladder, medial to pelvic sidewall
Boundaries
- Medial → Bladder
- Lateral → Obturator internus & pelvic sidewall
- Anterior → Pubic bone
- Posterior → Cardinal ligament
Contents (on lateral wall)
- External iliac vessels
- Obturator nerve & vessels
Surgical use
- Pelvic lymph node dissection
- Radical hysterectomy
- Access to obturator fossa
🟩 Pararectal space (MOST TESTED)
Divided by ureter
- Ureter = key landmark
▶️ Medial pararectal space (Okabayashi space)



Boundaries
- Medial → Rectum
- Lateral → Ureter
- Anterior → Cardinal ligament
- Posterior → Uterosacral ligament
Surgical value
- Nerve-sparing radical hysterectomy
- Hypogastric nerve identification
▶️ Lateral pararectal space (Latzko space)


Boundaries
- Medial → Ureter
- Lateral → Internal iliac vessels
- Posterior → Sacrum
Surgical value
- Internal iliac artery ligation
- Uterine artery ligation at origin
- Control of pelvic hemorrhage
5️⃣ Why pelvic spaces matter in surgery (EXAM GOLD)
🔑 Key principles
- Bleeding occurs when you leave the space
- Safe surgery = stay inside correct space
- Nerves & ureters lie in walls, not inside spaces
Applications
- Radical hysterectomy
- Pelvic lymphadenectomy
- Endometriosis excision
- Pelvic hemorrhage control
- Ureteric injury prevention
6️⃣ One-glance memory map (exam lock 🔒)
- Anterior → bladder related (Retzius, vesicouterine)
- Posterior → rectum related (Douglas, presacral)
- Lateral → vessels & nerves (paravesical, pararectal)
- Ureter divides pararectal space
- Presacral = dangerous bleeding
- Paravesical = lymph nodes
- Latzko = vessels
- Okabayashi = nerves